BY Amy Gonzalez, Managing Director, Strategy & Execution, & Dr. Matthew Weiss, Managing Director, EY-Parthenon, Ernst & Young LLP
BY Amy Gonzalez, Managing Director, Strategy & Execution, & Dr. Matthew Weiss, Managing Director, EY-Parthenon, Ernst & Young LLP
An improved hospital capacity management strategy can unlock value and boost financial performance.
 Many health system leaders remain financially cautious amid cost pressures and regulatory uncertainty. Hospital capacity management can establish an operational backbone, make health care networks more efficient, and improve cash flow and operating margins. It can also help systems differentiate themselves in the market.
Many health system leaders remain financially cautious amid cost pressures and regulatory uncertainty. Hospital capacity management can establish an operational backbone, make health care networks more efficient, and improve cash flow and operating margins. It can also help systems differentiate themselves in the market.
Implementation strategies in hospital capacity management will be unique and are influenced by system size, geography, technology adoption, staffing, governance, and proactive change management. Attention to these factors can not only improve financial performance but also impact patient experience.
How do hospital capacity management efficiencies impact free cash flow and operating margins?
Hospital capacity management involves the measurement of patient demand, patient conditions, building and bed capacity and other data that enable staff to predict patient needs and place people in the appropriate setting of care. Better management of resources, using technology and dedicated teams, allows patient throughput to increase. In addition, net patient revenue and operating margins can improve with the assumption that variable costs remain steady or decrease, and more patients fill beds. Improved margins create healthier free cash flow for systems, which is critical for systems facing financial constraints.
Just focusing on emergency room capacity can yield results. Of US health systems with a capacity management center that aimed to reduce emergency department boarding (holding admitted patients in need of inpatient beds), manage beds, and handle transfers, 72% tracked a positive level of financial return on investment (ROI), according to the Hospital Capacity Management Consortium, an American Hospital Association (AHA) unit formed in 2020.
Hospitals and health systems can focus on three areas — higher patient volume, lower variable costs, and better patient experiences — to achieve positive ROI from capacity management.
How can hospital capacity management increase patient volume and improve patient placement?
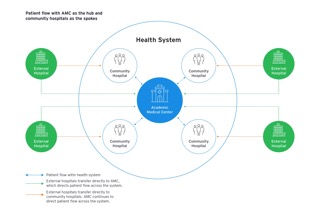
A proactive approach to patient placement based on need and appropriate setting, using real-time monitoring, allows health systems to load balance across the system and absorb additional patient volume. Capacity management can effectively improve patient volume and monitor capacity across hospitals by directing new patient volume into the system through the flagship hospital, community hospitals or external network, as well as through intra-network transfers for patients requiring different levels of care.
- A) Flagship hospitals and academic medical centers (AMCs) can benefit from the ability to transfer lower acuity patients to community hospitals. This will unlock capacity at the AMC that can then be backfilled with patients requiring more complex care. Further, community hospitals can benefit from a streamlined source of higher-volume, in-network patient transfers to increase bed utilization peripheral to the system hub or hubs.
- B) Community hospitals may also need to transfer patients to another facility for a higher level of care or due to capacity constraints. Retaining patients within the health system will offer enhanced continuity of care for the patient, reduce leakage and may financially benefit the system if filling an empty bed at one facility creates an opportunity to admit a new patient at the transferring facility.
- C) Capacity management strategies can also direct patient transfers from external hospitals to the health system. These patients could either 1) be transferred directly to the flagship hospital or AMC, with this hospital serving as a hub for patients and community hospitals as the spokes; or 2) be transferred to the community hospitals, with the flagship hospital or AMC decants from the community hospitals. (See Figure 1)
In addition to assessing patient needs and hospital occupancy, capacity management strategies can improve patient flow based on factors such as the availability of specialty care and specific procedures. A center of excellence or the establishment of hospital specialties can direct greater relevant patient volume to the appropriate location. Additionally, staff at these locations can work with inbound referral sources to expedite and streamline referrals for high-margin service lines in which the hospital may excel, such as cardiology or orthopedics.
How can hospital capacity management reduce operating expenses?
Health systems can proactively manage variable costs, including labor expenses, as a result of real-time capacity monitoring. For example, with improved monitoring of hospital capacity and patient flow, health systems can better staff at the right levels at the right time, ultimately reducing the need for costly overtime and unnecessary contract labor. Similarly, during peak illness seasons, systems will be quicker to respond and flex their staffing mix as needed.
Lastly, as hospitals enable and leverage technology for real-time monitoring of throughput and bed capacity metrics, they can streamline their operations to assess capacity across hospitals more efficiently. This approach saves valuable time and resources compared to contacting house supervisors at multiple facilities individually. The resulting faster and more coordinated clinical operations will simplify labor management and reduce labor expenses.
How can better hospital capacity management enhance health care quality and the patient experience?
Strategic patient placements and streamlined post-acute care coordination will also promote patient quality, satisfaction and experience, and expand access to care. Patients will be transferred between hospitals, ambulatory centers and post-acute facilities, ensuring they are transitioned to a site with the right staff, clinical and support resources, and equipment to best address their needs and enable safe and efficient access. This strategic and proactive approach to placement and coordination reduces readmission rates, ultimately reducing overall costs to serve the patient.
How does size, geography and operating model drive value creation from hospital capacity management?
- Strategic considerations
- Health system size and complexity: Large health systems may serve more diverse patient populations, clinical conditions and acuity. These factors necessitate health systems to allocate resources and time based on varying patient demands and treatment complexities. A capacity management center should also be able to coordinate patient transfers, admissions and discharges across multiple hospital and outpatient facilities, demanding standardized policies and procedures to manage patient flow effectively.
- Geographic region: Different regions may have varying patient demographics, healthcare regulations, market dynamics, resource availability and facility types (e.g., critical access hospitals), all of which impact operations and payer reimbursement models. Health systems must be able to adapt their strategies to ensure resources are allocated to meet specific patient needs while at the same time assessing the availability of healthcare resources, including staff, equipment and facilities.
- Operational factors
- Technology adoption: Data analytics and real-time monitoring of clinical operations and metrics, such as bed availability, patient acuity and average length of stay (ALOS), can enhance patient flow, inform forecasted patient demands and help predict capacity constraints.
- Staffing and resources: Effective capacity management staffing requires collaboration across a multidisciplinary team, including clinical roles, such as registered nurses with case management or critical care triage experience, patient flow physicians and ambulance dispatchers. The team also needs non-clinical members, such as data analysts, financial counselors and administrative support personnel.
- Outsourcing: For lean organizations looking to scale, capacity management activities, such as staffing the capacity management center itself and managing patient monitoring and placement, can be outsourced. However, outsourcing may reduce local operational control and decision-making ability. Health system leaders need to regularly assess these trade-offs to validate the appropriate financial and operational approach and should consider scenarios that account for changing conditions.
- Program design elements
- Governance and decision-making: Alignment on the reporting structure and decisions is essential for managing capacity. Clear escalation channels will be critical for timely and effective patient transfers and capacity management.
- Change management: Proactive management of operational change reduces employee resistance, ensures a smooth transition by leveraging a structured change management approach, enhances employee engagement and morale, and increases the likelihood of successful implementation.
Summary
Hospital capacity management can create financial value by lowering costs, improving margins and increasing free cash flow. System size, geography, technology, staffing, governance and other factors will make each hospital capacity management implementation strategy unique. In addition to financial benefits, better capacity management also can drive care improvements, and impact patient volumes and experiences, in a connected health care system.